She was absolutely, utterly exhausted.
It was the morning of Christmas Eve, and her kids, almost 4 and 2, woke her up “way too early,” excited for the holiday. A so-so night’s sleep didn’t help the fatigue that came on after a three-and-a-half hour drive to her parents’ home in Eastampton Township, Burlington County, the day before.
Christine Barmoy was 38 weeks pregnant.
Barmoy, a psychiatric nurse practitioner, took her own blood pressure. It was low. Very low. And she already knew she was dehydrated.
“I could barely stand up,” said Barmoy, 33. “My choice was to go to the ER on Christmas Eve or find someone to come to the house to give me an IV.”
She did a quick online search and found a company that offers “concierge mobile IV infusions.”
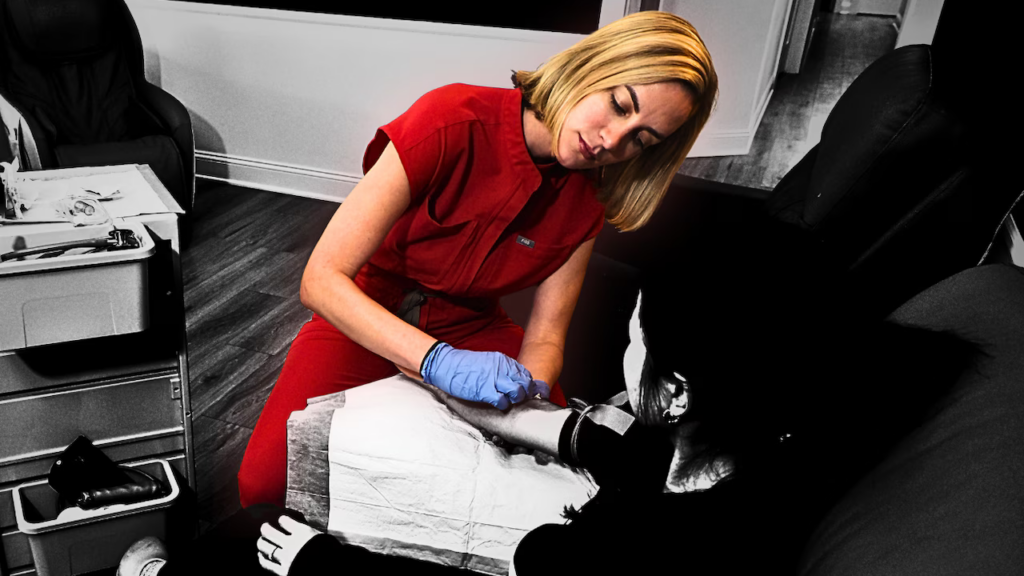
In an hour, a nurse was at Barmoy’s side, sticking a needle in her arm to deliver fluids with a little bit of sugar and electrolytes while keeping an eye on her vital signs.
“I could feel myself improving. And after, I felt back to normal,” Barmoy said of the $380 treatment, which isn’t covered by insurance. “It was worth every penny.”
IV drips are having a moment, thanks in no small part to celebrity endorsements. Everybody from Donnie Wahlberg – who created his own infusion concoction called “The Donnie” – to podcasterJoe Rogan have promoted these unconventional, semi-medical treatments that claim to cure everything from anxiety to a hangover.
But there’s one catch: Just who is putting the needle in your arm?
At the height of the COVID pandemic in April 2020, then-Gov. Phil Murphy signed an executive order that allowed Advanced Practice Nurses, or APNs, to run their own clinics and dole out medical treatments without a supervising physician. In the healthcare world, it was a huge change that supporters hoped would expand access to care when hospital systems and private practices were overwhelmed. Some nurse practitioners did just that. But others started their own “med spas” — hybrids between aesthetic medical centers and day spas — that offer non-emergency care like IV therapy and Botox.
The nursing community had been advocating for that kind of freedom and autonomy for decades.
But the result, critics say, is an industry that’s turned into a Wild West. Patients are receiving elective procedures that have serious risks – think tissue damage, nerve injury, serious allergic reactions or worse – in the back room of a fancified spa without a doctor in sight in case something goes wrong.
It’s unclear exactly how many nurse-run practices without a collaborating physician are in New Jersey. But one thing is for sure: they’re making money. Med spas alone across the state are earning between $1.3 and $1.6 billion a year, according to several industry estimates. And about 60% of the state’s more than 1,000 med spas opened their doors since COVID.
So it’s no surprise that nurses are now in the fight of their lives to keep control of their businesses.
In his last hours in office, Murphy lifted his COVID-era order, giving APNs only 30 days – until Feb. 16 – to either find a supervising physician or shut their doors. It sent the community into a tailspin.
“I need a lifesaver,” said Jenn Plescia, an APN who opened IVs By The Seas in Point Pleasant under the COVID rules. To stay in business, she will need to partner with a collaborating physician.
“We worked really hard to get here,” Plescia said, her voice cracking. “It sucks.”
She could catch a break from lawmakers, who have debated whether APNs should be allowed to practice independently since 2012. A state Senate version of a bill that would eliminate certain practice restrictions for APNs is set for a hearing on Feb. 9.
But getting a bill passed that fast – by the Feb. 16 deadline – is near impossible. And there is still no sponsor for the measure on the state Assembly side.
Gov. Mikie Sherrill declined to comment for this story. Unless she acts, the pre-COVID rules will kick back in. Med spas and other facilities run by APNs will need to close unless they get doctor sign-ons.
That’s exactly what should happen, some opponents say. Laws requiring doctors to oversee these medically-adjacent treatments are there to keep patients safe. They’ve had deadly consequences before.
A 47-year-old mother of four died after getting an infusion at a Texas med spa in July 2023.
“We don’t want nobody to go through what we went through,” the woman’s husband, Brian Cleveland, told a local television station last year.
“How many people got to die before we decide to do something?”
‘NO ONE IS DOING ANYTHING’
Drip. Drip. Drip.
The “Vitamin Sea Level 1” infusion was making its way into Plescia’s client’s arm while she panicked about her future.
(Costing $210 for an office visit or $275 for mobile delivery services, the mix is described as “packed with nutrients to help protect against infection, improve healing time, support your immune system and reduce the duration of illness.”)
“This is getting really bad,” she said before learning the APN legislation was up for a hearing. “No one is doing anything.”
In the three weeks since Murphy rescinded the COVID order, Plescia has been an incessant powerhouse on social media, railing against the 30-day countdown while promoting independence for practitioners like her.
She’s called lawmakers across the state. She’s tried to reach the governor.
She’s fighting for her spa’s life.
“This is like an ironman (triathlon race). Or ironwoman,” she said, noting that about 70% of practitioners who operate med spas are women.
“You have to swim. You have to get to the other side and I have sharks nipping at my feet,” said Plescia, 38. “I just need someone to send me a lifesaver so I can get on the other side.”
She said she worries about her clients, like the two teens who have been cyberbullied because of their acne but are showing progress — physically and emotionally — under her treatment. She worries about her 10 employees.
“A little prick. Relax. Pinch. Sorry,” she said, taking another moment with her client.
Her spa started as a side gig — she got her business license from the state in July 2021 — but her main job was still working in an emergency room.
But by that December, during a “horrible COVID wave where I was one nurse for 40 patients, I called my husband and said I couldn’t do it anymore.”
He encouraged her to quit and pursue her med spa business full-time. Within days of taking the jump, she got the kind of boost new businesses dream about.
On Dec. 26, 2021, Mike “The Situation” Sorrentino of “Jersey Shore” fame name-dropped Plescia’s business on Instagram, and the mention made its way into a People article: “Pretty serious situation right now,” Sorrentino wrote. “Day 4 with Covid 😐Thank you to @ivsbytheseas for that vitamin drip 💧 👌🏼.”
It was huge for her business, which she says has served more than 5,200 clients.
Plescia argues that throughout COVID, practitioners like her proved they could practice safely without a doctor in charge.
“Didn’t we show up, stepping up to the forefront during COVID under these executive orders — isn’t this a case study for how we can act autonomously?” she said.
She said she’s received offers from physicians and from private equity groups interested in buying her practice. She wants no part of it.
But she doesn’t really have a choice.
Before COVID, the rules about who can own a medical practice — and who can run one — were longstanding. So was the push for more autonomy for nurses.
In the 1990s, the rules for APNs, who used to work under stricter direction from doctors, transitioned to a less rigid collaboration model.
The idea was that the nurses and doctors would work together, and while APNs might manage their own patients, they always had a physician to consult when needed.
Collaborating physicians are more than partners on paper, experts say, adding they are legally required to be available for consultation and to review charts. They could also be held liable in lawsuits or board investigations.
While the COVID orders temporarily lifted the requirement for a collaborating physician, it never changed the rules governing who can own a medical practice.
Non-physicians can start a company and own the non-clinical side, but a physician has to own the medical service side — something that some med spa owners ignored when they set up shop during COVID. Nothing in the pending law would change that, so nurses still would not be allowed to own their own practices.
But those who have been running businesses since 2020 don’t want to fork over their lucrative profits.
“Here’s the thing,” Plescia argued about the doctor she’s now supposed to partner with.
“They don’t see or treat a patient, but they get all of the profits into their bank account?”
ARE THEY SAFE?
A tiny air bubble. The size of a grain of rice or soda fizz.Blink and you’d miss it.
But if it forms in the tubes used to infuse vitamins, fluids and other cure-alls into your bloodstream, it can float to your brain, heart or lungs and cause a heart attack, stroke or respiratory failure.
Other complications with the procedure can be deadly.
Jenifer Cleveland, 47, died after receiving an infusion of vitamin B and electrolytes at a med spa in July 2023. An investigation by the Texas Attorney General’s office is ongoing, but the state’s medical board determined a supervising physician failed to properly oversee treatment, which was administered by someone without a license.
“How many more other families have to go through this?” Cleveland’s widower Brian told a local reporter last year. “And you know, one is too many. Something needs to be done. So that nobody else ever has to go home and look at an 11-year-old little girl and tell her mother ain’t never coming home again.”
The death of the married mother of four inspired a new law in Texas that requires more supervision from a doctor for IV therapies.
A wrongful death suit filed by Brian Cleveland is ongoing.
It alleges “a cosmetic IV treatment became deadly when a national pharmaceutical distributor supplied hospital-grade electrolytes to an unqualified med spa operating without proper medical oversight,” Cleveland’s attorney, Matt Morrison, told NJ Advance Media.
“Jenifer Cleveland went in for IV vitamins and a spray tan and was dead less than half an hour later after a rapid potassium infusion.”
Warnings about elective IV therapy, questionable effectiveness claims and clinics that operate without supervising doctors pre-date Cleveland’s death.
In 2018, the Federal Trade Commission charged one IV seller with making deceptive promises about their IV cocktails’ abilities to treat cancer, congestive heart failure and multiple sclerosis. In 2020, it sent warning letters to other companies offering IVs to fight the coronavirus.
And the Food and Drug Administration warned in 2021 that some med spas and IV clinics were mixing products inappropriately without proper sterilization. “Contaminated, or otherwise poor quality, compounded drug products can lead to serious patient illnesses, including death,” it said.
While there have been no elective IV deaths in New Jersey, plenty of med spas have come under scrutiny for performing procedures without proper authority.
A Passaic County spa owner in 2024 agreed to pay $10,000 and was banned from skin care for 10 years after operating without a medical license. The state found Rasha Abdul N. Basuf, the owner of the now-defunct Skyn Spa in Clifton, illegally performed procedures including Botox, dermal fillers, laser hair removal, microneedling, “vampire facials,” body contouring and teeth whitening.
In 2025, the license of a massage therapist was suspended for five years after she was accused of performing procedures that went beyond the scope of her license. Ana C. Velazco, who owned and operated Fabsilhouette – also known as Medical Massage Network – in Fair Lawn was permanently barred from owning or operating a massage business or med spa after the state said she gave fat‑dissolving injections, performed microneedling and removed post‑surgical sutures.
That’s exactly why some doctors say it’s time for the COVID rules to go.
CHANGING THE RULES?
Let Florida be a “cautionary example,” said Claudine Leone, an attorney for NJ Government Affairs Counsel, a lobbying group representing several physician associations.
Nurses and their allies say APN autonomy increases access to care in underserved populations. But a 2025 study in Florida found of 328 independent nurse practitioner practices in the state, only 128 provided primary care.
“Despite Florida law limiting independent practice to primary care, nearly 60 percent were operating cosmetic, aesthetic, IV hydration and other cash-based practices,” Leone said.
“APNs are not automatically drawn to underserved communities or high-need care. They are drawn to profitable, low-complexity, cash-based services.”
New Jersey saw similar changes under the COVID orders, with APNs leaving hospitals and primary care practices to open non-traditional practices like med spas.
Among the side effects, doctors say, is patients receiving the wrong treatments, ones that don’t work, or that they don’t need – and paying out of pocket for all of it.
Rahul Vemula, a board certified plastic surgeon who is also vice president of the New Jersey Society of Plastic Surgeons, told a story of a recent patient who went to a med spa without physician oversight.
The patient wanted to get rid of excess fat in her belly and paid for CoolSculpting, a non-surgical procedure that freezes and destroys fat cells. It’s FDA-approved but not covered by insurance.
“If this patient had gone to a plastic surgeon, she immediately would have been told that the non-surgical treatment would not achieve her goals,” said Vemula, who is based in West Long Branch.
She needed an abdominoplasty, commonly called a “tummy tuck,” he said.
“One thing that she said to me really stood out. `I never saw a doctor and I thought they knew what they were doing,’” Vemula said of his patient. “The harm here was that a patient spent thousands of dollars for a treatment that should not have been performed and failed to achieve her goals.”
But state Sen. Joseph Vitale, D-Middlesex and co-sponsor of the bill, said nurse practitioners across all disciplines proved themselves during COVID.
He called giving them independence a “game-changer” and said med spas and more traditional practices can both be run by nurses.
“We have a workforce shortage in healthcare,” said Vitale, chairman of the Senate health committee.
“I couldn’t really care less about the very basic cosmetic elective procedures. … If someone wants to have plumper lips, God bless,” he said. “I want kids to get pediatric care and people to get mental health services.”
If Vitale’s bill doesn’t pass, some nurses said, they’ll be taking their services elsewhere.
Cara Carpin left family medicine and opened Restore Health by Science in Marmora in 2023 under the COVID rules.
She treats as many as two dozen clients a week with hormone therapy — through injections or oral capsules — to treat everything from menopause and erectile dysfunction to decreased libido and depression.
“The reality of what this means is staggering,” Carpin said. “I am now being forced to pay a physician simply to satisfy a regulatory requirement, even though that physician will not treat patients in my clinic, may never step foot in the building, and doesn’t even need to live in New Jersey.”
If she can’t keep her practice here, she says she’ll move it to Maryland, a state where it’d be allowed to operate with fewer restrictions.
Marcel Kaganovskaya, a family and psychiatric-mental health nurse practitioner who works in Montclair and New York City, is also questioning whether he will continue to practice in New Jersey.
“It’s very stressful,” said Kaganovskaya, who also is the executive director of The Society of Psychiatric Advanced Practice Nurses.
Adding a collaborating physician to his practice — a person who would not see patients and may never enter an exam room — could cost from $1,000 to $2,000 a month, he said.
“This is going to be a public health emergency,” he said, worrying that many practitioners may leave the state if they can’t practice independently.
Plescia said she keeps working – both with her clients and on the phones to anyone who will listen – but she can’t stop looking at the calendar.
“Sometimes I just feel New Jersey hates nurses,” she said.
NJ Advance Media reporter Jackie Roman and Research Editor Vinessa Erminio contributed to this report.
SOURCE: https://www.nj.com/news/2026/02/is-there-a-doctor-in-the-house.html
